All About Labor Induction
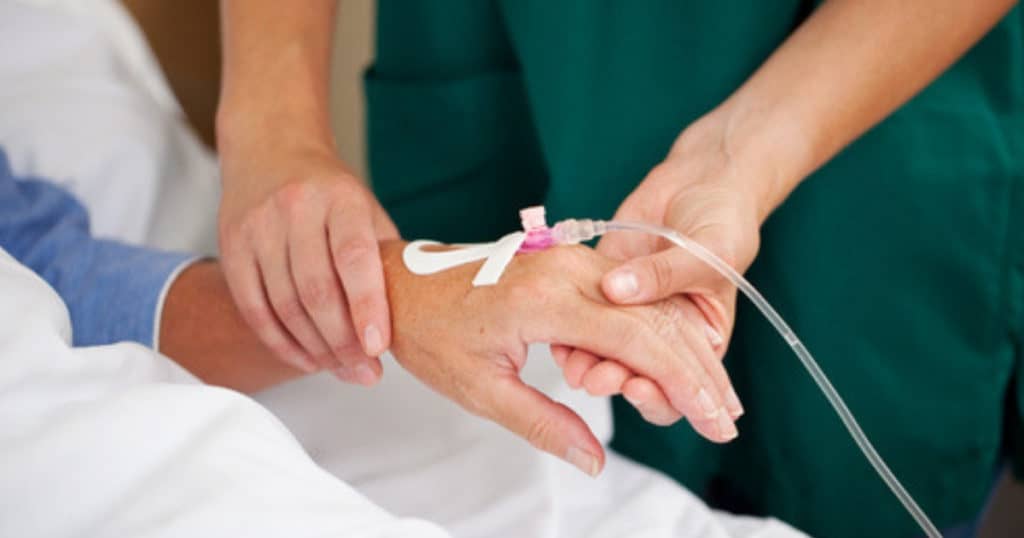
Labor induction is the process of using medical interventions to stimulate labor.
When it comes to starting labor, it’s generally recommended to wait for it to begin naturally, unless there are specific medical reasons that call for induction. Some reasons given for induction include: hypertension, preeclampsia, heart disease, gestational diabetes, infection in the uterus, placenta complications or other medical complications.
What happens in an induction?
Some of these steps may vary depending on the protocol and policies of the care provider, place of birth or how ready your body is for labor:
1. IV fluds:
Your nurse will administer an IV and you will begin receiving fluids.
2. Electronic fetal monitoring:
Electronic fetal monitors will be placed on your belly to measure the baby’s heartbeat and any contractions.
3. Cervix ripening:
If your cervix is not yet effaced, a ripening agent (synthetic prostaglandin) may be used. You may be given the medicine orally or it can be placed directly in your vagina to stimulate the effacement or thinning of your cervix. Another option is a foley catheter. A thin tube is placed in your cervix with two very small uninflated balloons at the end. The balloons are inflated with a saline solution and this stimulates effacement and dilation. Once your cervix dilates to around 3 cm, the catheter falls out. How long this step will take depends on how effaced you are to begin with. It could be just a couple of hours or it may be done overnight while you sleep in the hospital with the aim of putting you into labor by morning.
In some cases this step is all that is needed to get labor going and start contractions. When this happens, you may not need further interventions and will continue laboring on your own.
4. Pitocin:
If you arrive to the hospital and your cervix is already ripe, your OB or midwife may decide to administer pitocin, the synthetic version of the hormone oxytocin, through your IV immediately. The pitocin drip begins at a low dosage and it is increased or decreased as needed based on how your body responds. The purpose of the pitocin is to bring about regular contractions in your uterus that result in dilation. You will notice the sensation of a tightening in your uterus and this will happen in a regular pattern. As the pitocin dosage is turned up, the contractions will get stronger and more intense.
5. Vaginal exams:
Your care provider will do routine cervical exams to see how far dilated and effaced you are and make adjustments accordingly.
6. Rupture of membranes:
Your doctor or midwife may suggest rupturing your membranes if this has not already happened. Your provider will use a small hooked instrument, place it through the cervix and break the amniotic sac.
7. Internal fetal monitoring:
If the nurses are having a hard time keeping the baby on the monitor, you are high-risk or the baby is not responding well to the contractions, your birth team may want to use internal fetal monitoring to get a more accurate measurement. To do this, your membranes must be ruptured. A fetal scalp electrode is screwed directly into the top layer of skin on your baby’s scalp, which then relays your baby’s heart rate to the fetal monitor. Additionally, an intrauterine pressure catheter (IUPC) may be placed inside the uterus between the uterine wall and the baby. This measures the strength of your contractions.
8. Labor pains:
In our experience, some women have a harder time coping with the contractions brought on by an induction than they do with spontaneous labor contractions. Lack of ease of mobility may be a contributing factor. In many cases, an epidural is requested if the discomfort of the contractions becomes too great. Read more about what it is like to have an epidural here. Some women do not request an epidural and choose to cope with the labor pains using other methods such as breathing, hypnobirthing, their labor support team and nitrous oxide.
9. Birth:
Once you have a steady, effective labor pattern, your OB or midwife may stabilize the pitocin dosage and you will continue laboring until you are fully dilated and ready to transition into giving birth.
To learn more about the evidence for inductions on the following topics we recommend checking out these articles from Evidenced Based Birth:
Induction for Going Past Your Due Date
